
CONDITION
Abnormal Uterine Bleeding (AUB)
Heavy, irregular, or prolonged bleeding can signal underlying conditions like fibroids, hormonal imbalance, or endometrial issues. Dr Michael Wynn-Williams offers thorough investigation and personalised treatment, including surgical options where appropriate.
What is Abnormal Uterine Bleeding?
AUB describes any bleeding from the uterus that is different from your normal menstrual pattern. This includes changes in how often, how long, or how heavily you bleed, as well as bleeding at unexpected times.
Normal menstruation typically occurs every 24–38 days, lasts up to 8 days, and involves a blood loss of around 5–80 mL per cycle. AUB is bleeding that falls outside this range and affects your daily life, physical health, or emotional well-being.
Does AUB mean I might have cancer? The vast majority of cases are due to benign (non-cancerous) causes such as fibroids, polyps, or hormonal changes. However, it is important to investigate properly — particularly postmenopausal bleeding or a thickened uterine lining — to rule out endometrial cancer or pre-cancerous changes. Prompt investigation provides reassurance and, if needed, early treatment.

Types of Abnormal Bleeding
Heavy menstrual bleeding (HMB): Periods that are unusually heavy or prolonged — soaking through pads or tampons quickly, passing large clots, or bleeding that disrupts normal activities.
Intermenstrual bleeding: Bleeding between periods, including after sex (postcoital bleeding).
Irregular periods: Cycles that are unpredictable in timing or length.
Postmenopausal bleeding: Any vaginal bleeding occurring 12 or more months after your last period requires prompt investigation.
Prolonged bleeding: Periods lasting more than 8 days.
Heavy menstrual bleeding affects roughly 1 in 4 women at some point in their lives. Despite being very common, many women suffer in silence, assuming it is simply a normal part of life. It is not something you need to put up with — effective treatments are available.
When Should You Seek Help?
You should see your GP or a gynaecologist if:
Your periods are so heavy they disrupt your daily life or work
You need to change pads or tampons more often than every 1–2 hours
You regularly pass blood clots larger than a 50-cent coin
You bleed between periods or after sex
You bleed after menopause (any bleeding after 12 months without a period must be investigated)
You feel unusually tired, short of breath, or faint — which may suggest iron deficiency anaemia
Seek urgent medical care if:
You are soaking through a pad or tampon every hour for two or more consecutive hours
You feel dizzy, faint, or have a racing heartbeat
You experience sudden, severe pelvic pain with bleeding
You think you may be pregnant and have bleeding with pain
Go to your nearest emergency department or call 111.

Treatment Options
Treatment depends on the underlying cause, the severity of your symptoms, your age, and whether you wish to preserve your fertility. There is no single right answer — the best approach is one that fits your individual circumstances and preferences.
Medical (Non-Hormonal) Treatments
Tranexamic acid: A non-hormonal tablet taken during your period that reduces blood loss by around 40–50%. It does not affect your fertility.
NSAIDs (e.g., mefenamic acid, ibuprofen): Reduce blood loss and help with period pain.
Iron supplementation: Oral or intravenous iron replacement if anaemia is present.
Hormonal Treatments
Levonorgestrel-releasing IUCD (Mirena): A small device inserted into the uterus that releases a low dose of progestogen locally. It is the most effective long-term medical treatment for heavy menstrual bleeding and is widely used in New Zealand. It also provides contraception.
Combined oral contraceptive pill (COCP): Regulates and lightens periods in many women.
Progestogen tablets or injection: Can help regulate irregular cycles and reduce bleeding.
GnRH analogues: Used in specific situations (e.g., prior to surgery for fibroids) to temporarily stop periods and reduce fibroid size.
Surgical Treatments
Hysteroscopic polypectomy or myomectomy: Removal of polyps or small fibroids through the cervix — no cuts to the abdomen. Suitable for women with polyps or submucosal fibroids.
Endometrial ablation: Treatment of the uterine lining to significantly reduce or stop periods; a day procedure for women who have completed their family and do not want major surgery.
Laparoscopic myomectomy: Keyhole removal of larger fibroids while preserving the uterus — suitable for women wishing to retain fertility.
Uterine fibroid embolisation (UFE): A radiological procedure that cuts off the blood supply to fibroids, suitable in selected cases.
Hysterectomy: Surgical removal of the uterus, performed laparoscopically (keyhole) where possible. Considered only when other treatments have not worked or are not suitable, and when your family is complete.
Your preferences matter. Research consistently shows that the most important factor in managing heavy bleeding is how it affects your quality of life — your work, relationships, and daily activities. Dr Wynn-Williams will work with you to find a solution that suits your life.


Dr Michael Wynn-Williams
MBChB (Otago), FRANZCOG
Gynaecologist, Advanced Laparoscopic Surgeon, Endometriosis and Pelvic Pain Specialist
Dr Michael Wynn-Williams is a highly experienced Auckland gynaecologist and laparoscopic surgeon, specialising in the treatment of endometriosis, fibroids, pelvic pain, and ovarian cysts. With a commitment to minimally invasive surgery and evidence-based practice, he helps women across tNew Zealand achieve better outcomes with empathy, precision, and respect
-
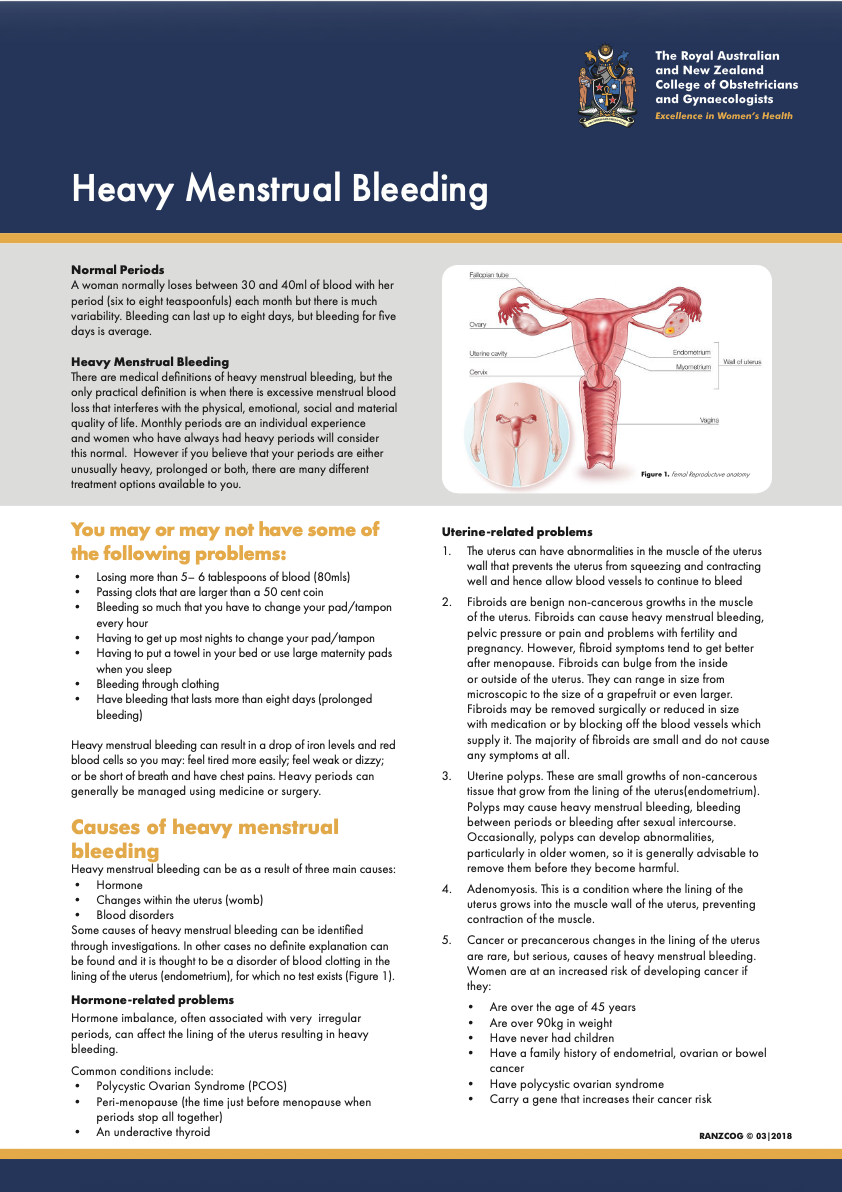
RANZCOG Heavy Menstrual Bleeding Information Sheet
-

Mirena IUCD Information
-
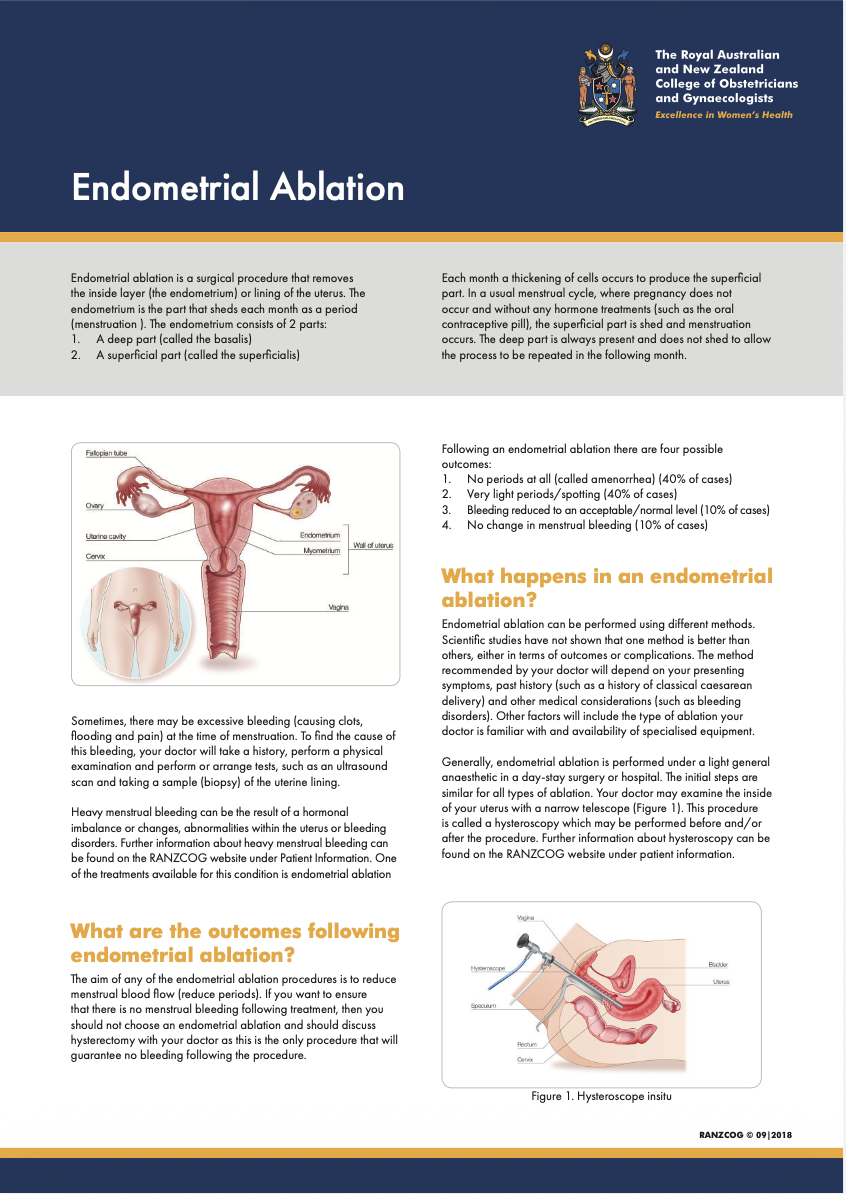
RANZCOG Endometrial Ablation Information Sheet
